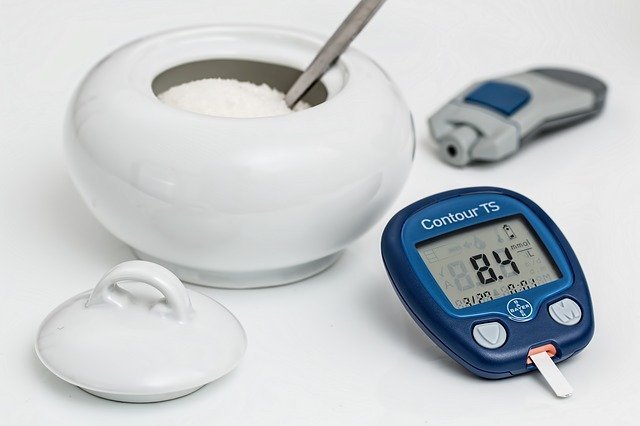
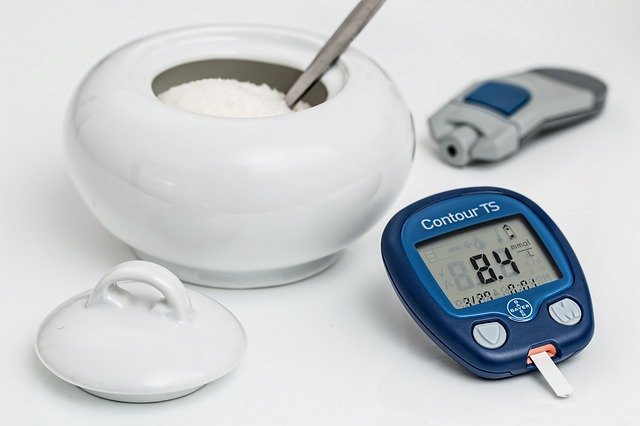
Diabetes – definition, symptoms and treatment
Epidemiology
In France more than 90% of people with this disease have type 2 diabetes. To Prevalence rises with Old and most commonly occurs around the age of 50. This prevalence is higher at the same age high in men than in women. Over the last ten years, the number of people treated has increased by an average of 5% per year.
Causes of diabetes
The increase in the number of people affected is due to the quality of the diet. Actually it is Increased consumption of sugar, bad fats and alcohol contributes to an increase in risk factors. In addition, there are health-damaging behaviors such as lack of exercise or smoking creates a breeding ground in our body for the development of various chronic diseases.
In addition, these are advanced patients Age, being In Surcharge Weight or obesity, which trigger type 2 diabetes.
Memories: Glucose
Glucose is a food energy. It is stored in the form of in the liver and muscles Glycogen. The blood sugarin other words the tblood sugar levelis regulated by the secretion of a hormone pancreas First name insulin. The latter represents the clef what does that enable? glucose penetrate the cells of our body. Elle inhibits the availability of glucose and promotes its storage.
How pathology works
Stadium 1
After taking a meal, Beta cells of the islets of Langerhans in the pancreas secrete Insulin. The latter enables that Distribution of excess blood sugar to the body’s cells. For a diabetic, that is insulin resistantl’Fat accumulation in fatty tissue can occur flammable. The Lipotoxicity will trigger that Production of fat cells.
These transmit inflammation into the blood and promote intestinal porosity. The inflammation chronic will disrupt the blood sugar regulation process decreased sensitivity to glucose. This creates insulin resistance. This phase is referred to as Pre-diabetes and maybe modifiable by practicing a physical activity and in make a change in diet.
Stadium 2
phase irreversible in the progression of this pathology. The amount insulin is produced by the pancreas doubled to regulate them abnormal blood sugar concentration. The insulin-producing pancreas becomes exhausted. It follows a Sugar intolerance due to lack of insulin secretion.
Signs of the disease
The Screening is generally performed during a Routine check. Apart from the complications caused by the pathology, this is indeed the case minimally symptomatic. Clinical signs associated with overweight or obesity are important for screening.
Polyuro-polydipsic syndrome
THE Signs and symptoms of type II diabetes are dominated by what is called Syndrome polyuro-polydipsique. The Polyuria This is nothing but a fact urinate frequentlyT. This leads to polyuria large water losses causes that Polydipsia characterized by The thirsty WHO increase.
weight loss
We also observe a weight loss in patients in the discovery phase and a tendency towards this Polyphagia. Polyphagia is characterized by A hunger exaggerated with Lack of satiety. When patients are very hungry, they eat a lot without necessarily gaining weight.
Asthenia
As a result of this weight loss follows a Asthenia or severe fatigue accordingly a improper use of carbohydrates from food. Added to this is the Tissue protein loss.
Excess weight is on the waist belt
Two of these are overweight or obesity, which are characterized by a fat mass on the abdominal belt Factors that promote type 2 diabetes.
With
If you notice some of these signs, there is no need to worry quickly. It is recommended to seek the advice of your doctor who will carry out the examinations necessary for the diagnosis.
Generally, we only notice the appearance of these signs when the fasting blood sugar level exceeds 3 g/L, so we sometimes diagnose the disease a little too late.
In fact, when triggered after several years of blood sugar resistance, he cannot heal himself. On the other hand, care remains important to avoid the associated complications (infections, cardiovascular accidents (CVA), myocardial infarction, hypertension, amputations, etc.).
diagnosis
Hyperglycemia
The measurement of the Blood sugar is a Examination that confirms the diagnosis of diabetes. It is a measurement tool most often used as a first intention. In fact, the latter gives us one Immediate feedback on the status of blood sugar concentration.
Below are the threshold values that determine the diagnosis:
- Fasting blood sugar > 1.26 g/L
- Blood sugar > 2g/L at any time of day
- 1.1 < glycemia < 1.26 : We can assume a Glucose intolerance. For these patients we practice a oral glucose tolerance test (TTOG, HPOG-induced oral hyperglycemia).
Read right
The Capillary blood sugar or “dextro” as part of the monitoring of this pathology Collection of a drop of capillary blood from the fingertip. Blood is deposited on glucose reductase strips. Reading is done by a device called Blood glucose meter.
Dosage of glycated hemoglobin
Another discovery method is possible thanks Blood test for glycated hemoglobin. The latter results from the Fixation of a glucose molecule on globin chains. This dosage is nothing other than the rEffect of blood sugar control in the last 3 months. So it gives us information about the regularity of blood sugar levels over several weeks before the examination. The normal value of glycated hemoglobin is less than 6%. To avoid complications, The goal for diabetics is not to exceed 7%.
Glycosuria
Glucosuria is characterized by the presence of Sugar in urine. His appearance is associated with a Blood sugar level too high. At healthy subjects she is strict zero.
Ketonuria
Ketonuria is represented by abnormal presence of ketone bodies in the urine. We use test strips that detect thisAcetoacetate. If the test is positive, diabetes is not systematically present.
Insulin and C-peptide dosage
These dosages allow the distinction between type I and type II diabetes. They are carried out as part of a induced oral hyperglycemia. A Low or no insulinemia that shows no variation suggests type I.
Yes, yes The C-peptide dosage is lower than standard: 0.8 g/LThis confirms insulinopenia. That means that the Insulin production is inadequate or even absent. What causes this form to occur?. The C-peptide allows the a and b chains of insulin to be linked as it ensures the transport and folding of insulin in the cells of the pancreas.
Complications
The complications of type 2 diabetes are numerous. On the one hand, we can divide them into two parts acute complications and on the other hand the chronic complications.
Acute complications
- Hypoglycemia: malaise, headache…
- Hyperosmolar decompensation (dehydrated elderly, hyperosmolarity, hyperglycemia and glycosuria).
- Lactic acidosis (metabolic acidosis: pH < 7.38 due to lactate accumulation)
Chronic complications
- The macroangiopathies : atherosclerotic plaques in the large vessels of the heart (angina, infarction), brain (stroke, TIA), legs (PAAD: obstructive arteriopathy of the lower extremities).
- Microangiopathy : in small vessels, eyes (retinopathy, cataracts), kidneys (nephropathy, renal failure), nerves (diabetic neuropathy).
Hypoglycemia
Although the main feature of type 2 diabetes is hyperglycemia, Hypoglycemia is also one of the most common complications observed in diabetics. Hypoglycemia is characteristic less than 0.6g/L. The symptoms are specific; Paleness, trembling, sweating, racing heart, sweaty hands, severe hunger, blurred vision, tiredness, dizziness and finally difficulty concentrating…
In addition to the previous symptoms, hypoglycemia may worsen by then Coma, seizures, possible falls or traffic accidents while driving, stress attacks that can lead to stroke or heart attack.
Which treatments?
Urgent case of hypoglycemia
On a conscious topic
During hypoglycemia, the first action for a conscious person is to do the following: Stop any ongoing physical activity. Secondly, the patient must be sweetened with 15 grams of sugar, which is equivalent to three sugars or a glass of fruit juice. We leave it up to action ten minutes then we offer the patient a meal or snack. Blood glucose is checked 15 minutes after hypoglycemia to ensure stability.
On an unconscious topic
In the event that the person is unconscious, this is necessary immediately Repeat first aid measures by placing the patient in a side safety position. If possible, blood sugar will be measured. We injected glucagon (molecule with the opposite effect of insulin) intramuscularly and we call it Samu.
Oral medications
Apart from changing the diet, the patient sees himself prescribe oral antidiabetic drugs which are of different types:
- With insulin resistanceRecipe from BiguanideMetformin as initial treatment. Especially if the patient is overweight. The treatments help glucose enter cells.
- In case of an increase of Insulin secretionPrescription of sulfonylureas and glimides.
- During the decreased absorption of glucose at the digestive levelPrescription of an inhibitor of Alpha-glucosidase.
- When oral treatments no longer work and to reproduce pancreatic secretion, we use them Injection of TTT or insulin in two forms. On the one hand, that bolus to cope with food intake. On the other hand, that is basal so that the body can function. The key is to check that the basal rate meets the patient’s basic needs. This is what it is necessary forInform people to adjust their dosage, self-monitor their blood sugar levels, and vary injection sites to avoid lipodystrophies.